Healthcare consumers are just as likely to factor in convenience as they do cost when deciding where to seek care and from whom, according to a new survey of 4,037 American adults about their attitudes and preferences as patients.
The survey, conducted from April 19-28 by JLL, in many ways confirms the obvious: that older generations seek preventive care more often than younger generations; that insurance coverage is a primary driver for choosing a provider or hospital; and that the quality of service affects the patient experience.
Nearly eight of 10 of the survey’s respondents had received at least one type of non-dental care in the last year. Women, who accounted for 51% of the survey’s respondents, are more likely to receive care overall, but men are more likely to receive emergency care.
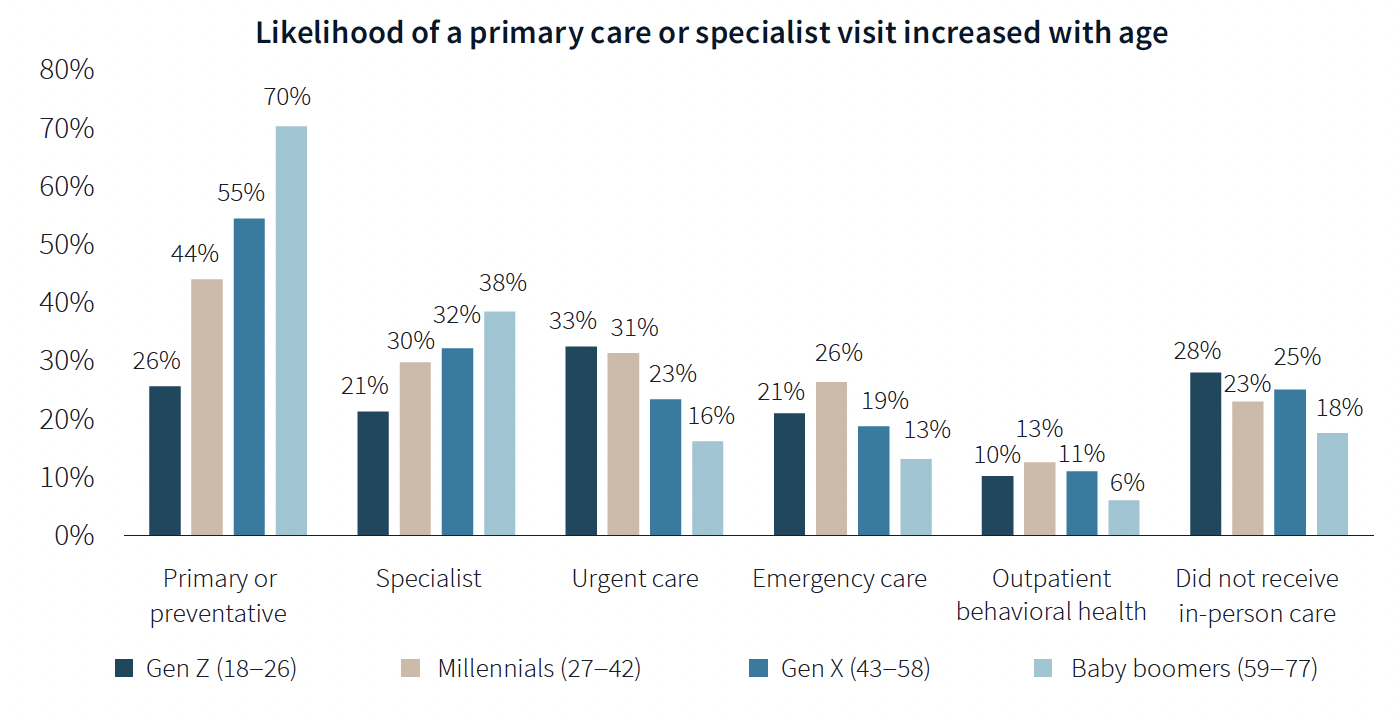
The likelihood of a primary care or specialist visit increases with age: 80% of adults 65 years or older have two or more chronic conditions that require continuous care. More than 70% of Baby Boomers (who accounted for 29% of the survey’s respondents) had received primary or preventive care within the last year, compared to only 26% of Generation Z.
Younger generations are more reactive than preventive in their healthcare decisions, borne out by the survey’s finding that Millennials and Gen Zs (43% of the survey's respondents) are more likely to receive urgent care, emergency care, and outpatient behavioral healthcare than older adults.
Proximity to patients counts
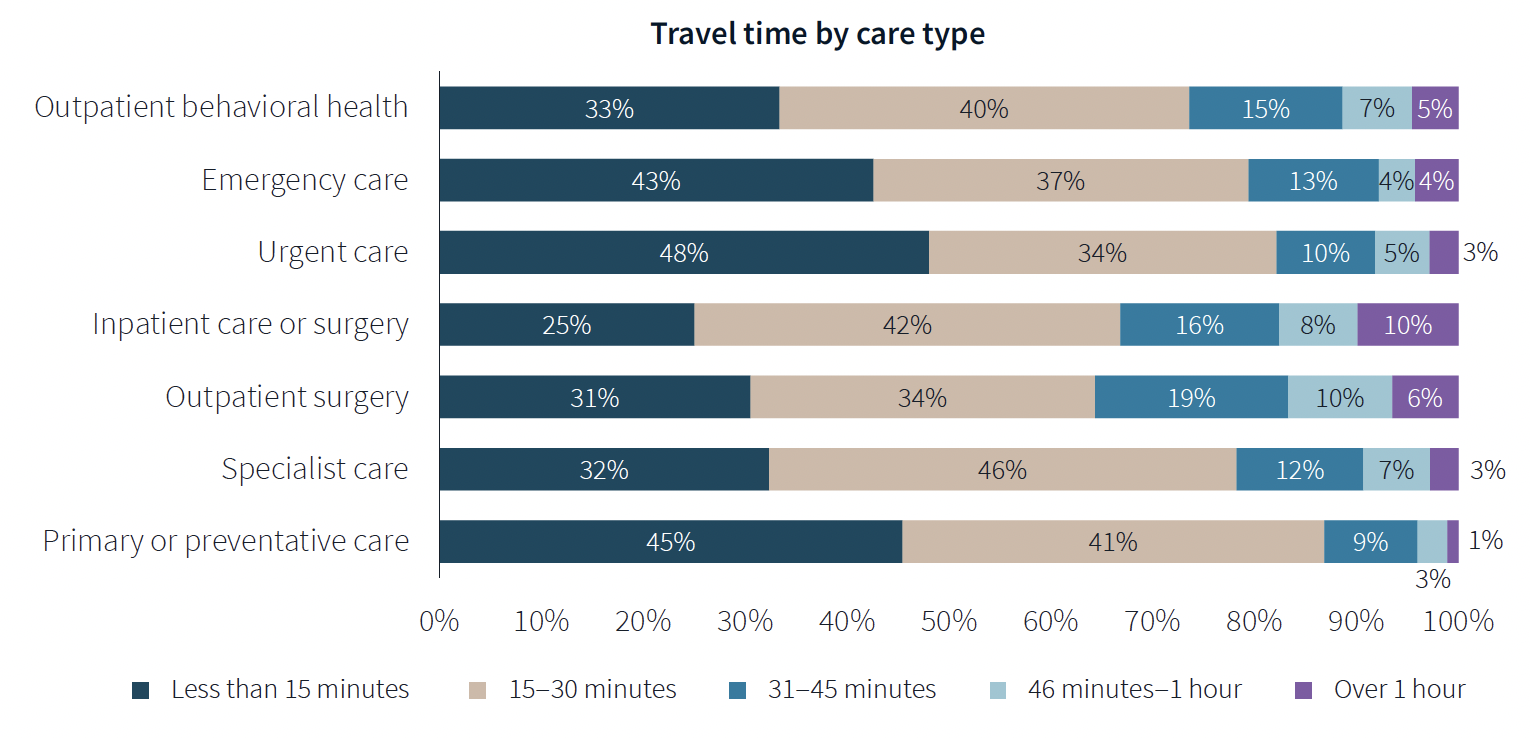
When care is urgently needed, “decision factors are simplified,” the survey states, and location and proximity of care are ranked higher as decision-making factors. But even outside of emergencies, convenience ranks high among factors for patients seeking care.
There’s no denying that cost is always in the background of any healthcare decision. “Accept my insurance” was the most common factor for choosing a provider among the survey’s respondents. (82% of participants has private insurance, and 81% has public insurance.)
Two-fifths of respondents said they travel less than 15 minutes to receive care, and nearly eight of 10 respondents travel less than 30 minutes. Among those with appointments in standalone medical offices, 85% ranked location as convenience, which the survey suggested indicates the advantages of a dispersed location strategy.
“A strong location strategy can improve reach for health systems and physician practices and potentially improve care outcomes,” JLL writes. “But there is a balance between convenience and cost—health systems need to balance the benefits of being close to their target population with the cost of a new facility or doctors’ time in transit from a local clinic to the hospital.”
Convenience is also key both in location and in being able to navigate to care. Patients want to get to care quickly and get on with their day. Ease of parking and ability to navigate the facility also affected a facility’s net positive score in the survey.
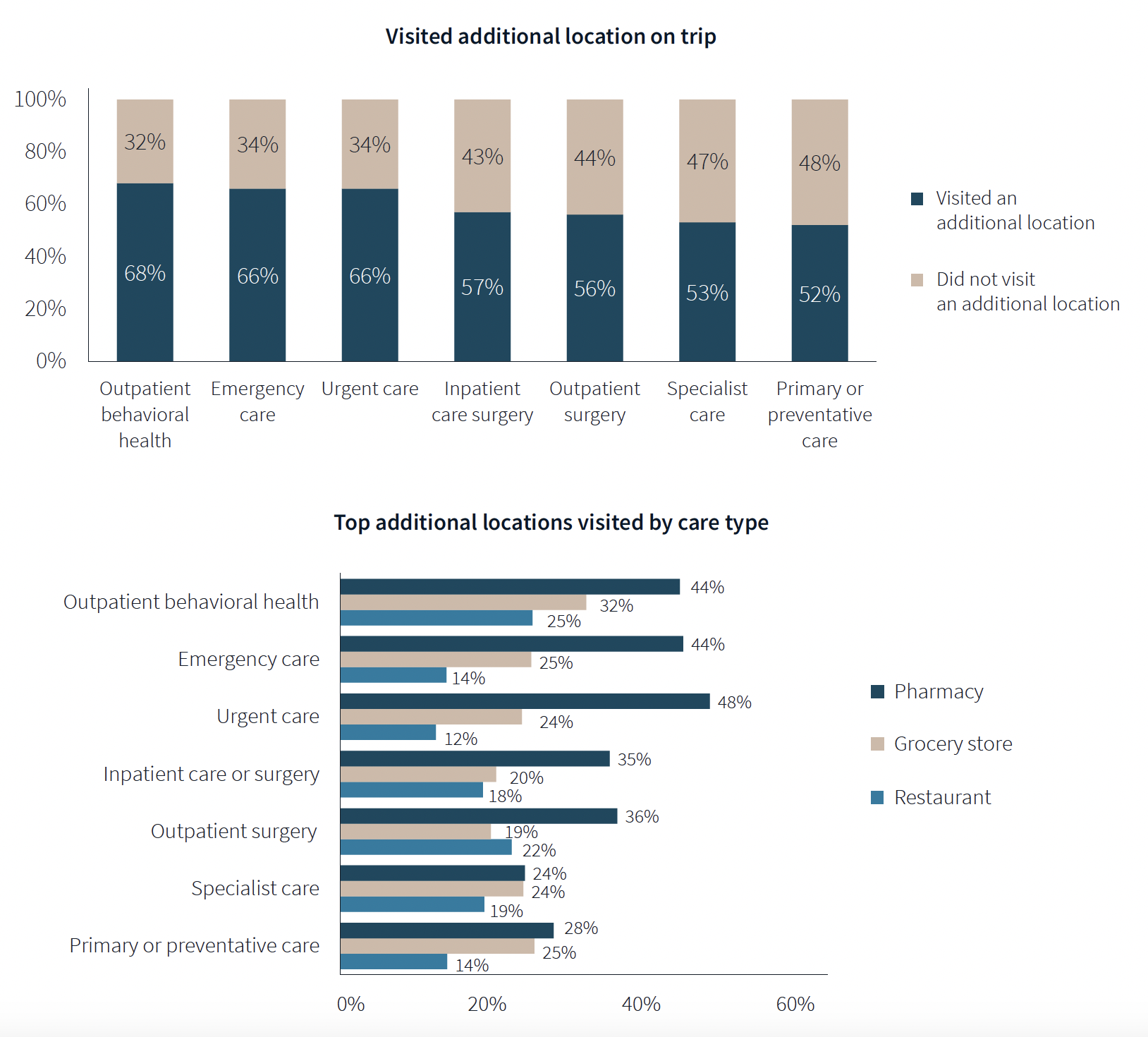
One of the survey’s more revealing findings is that nearly three-fifths of respondents—58%—went to another location—such as a pharmacy, or an urgent clinic—as part of their trip for healthcare.
Word of mouth often defines quality of care
Patients seem to be open to diverse care choices. For example, 29% said they have visited a retail clinic, such as a CVS, and would do so again. Gen Z and Millennials are more likely to frequent retail clinics for their convenient appointment schedules and shorter wait times.
More than two-fifths of respondents—42%—had a telehealth appointment within the last year, which was slightly down from the 45% in JLL’s 2022 survey. This year’s poll also found that 29% of telehealth appointments led to an in-person visit.
More than 40% of respondents ranked “reputation of quality” among the top five factors for choosing care. But where they get their impressions about quality varies.
Referrals play a larger role in specialist, outpatient surgery and inpatient care. Recommendations from friends ranked most highly for behavioral health, given the personal nature of such care, and was ranked in the top five by 31% of respondents. Younger patients, who “have yet to develop brand loyalty,” according to the survey, are more likely to rely on word-of-mouth recommendations than older patients for whom hospital systems’ reps matter more.
Outpatient surgery and primary care ranked highest for provider satisfaction; emergency care ranked lowest. Participants ranked their experiences on 12 aspects of care, and the biggest gap between “promoters” and “detractors” was for the service level of providers. Primary care had the highest net provider score, with 86% of respondents ranking its care as “attentive.”
Some amenities draw patients
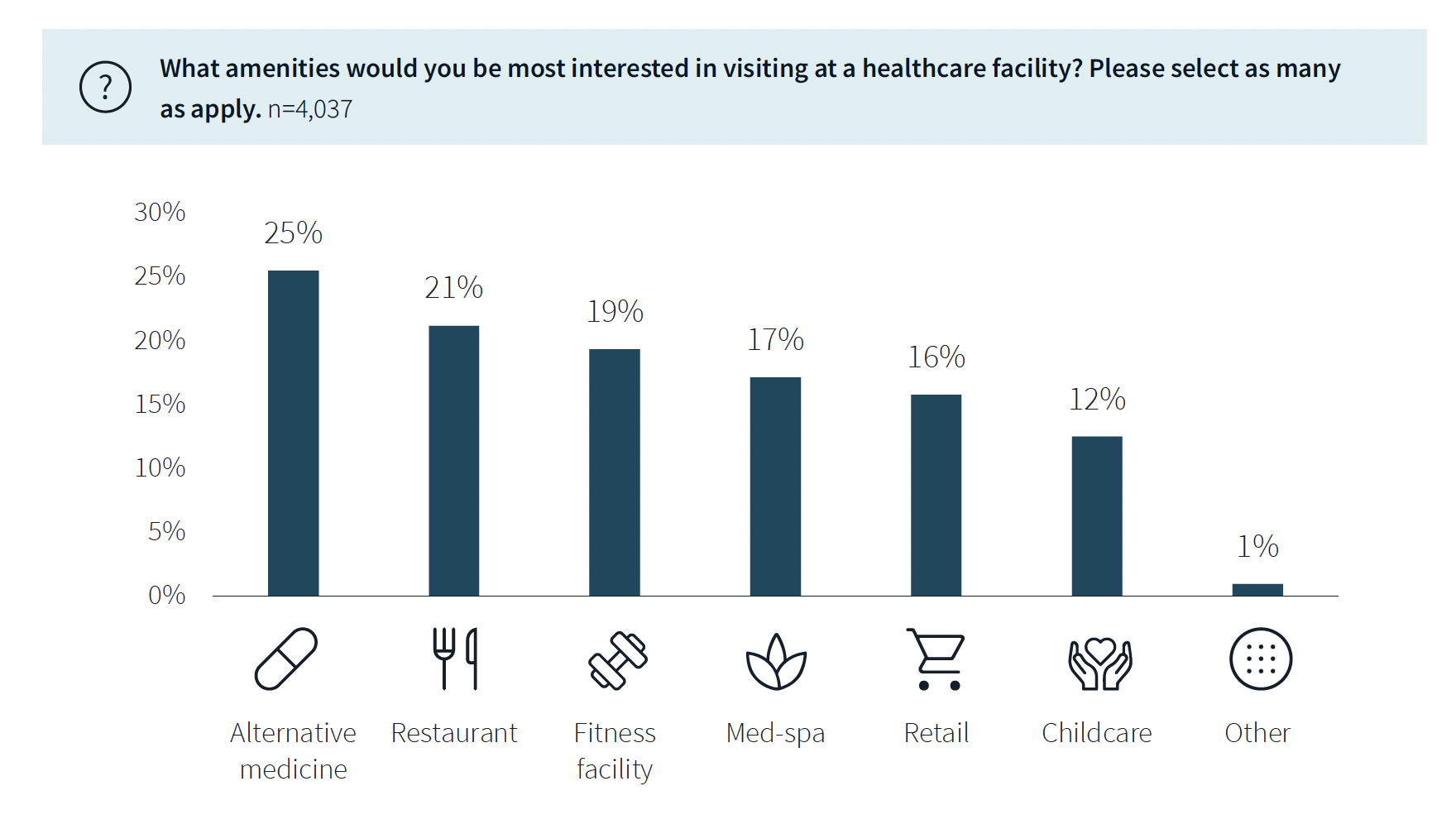
While not a decision-making factor, amenities do attract some patients. Among the survey’s respondents, 63% said they would be interested in visiting a healthcare facility with an additional amenity, such as alternative medicine, a restaurant, fitness center, or spa. (This inclination was more evident among younger respondents.)
The overall quality of facilities, including the comfort of their waiting rooms, can impact a patient’s choice, especially for inpatient, urgent, and emergency care. The survey also found that urban locations have lower favorability rankings for their facilities, signaling room for improvement. (Just under half—48%—of respondents live in the suburbs.)
Related Stories
Coronavirus | Apr 10, 2020
COVID-19: Converting existing hospitals, hotels, convention centers, and other alternate care sites for coronavirus patients
COVID-19: Converting existing unused or underused hospitals, hotels, convention centers, and other alternate care sites for coronavirus patients
Coronavirus | Apr 9, 2020
COVID-19 alert: Robins & Morton to convert Miami Beach Convention Center into a 450-bed field hospital
COVID-19 alert: Robins & Morton to convert Miami Beach Convention Center into a 450-bed field hospital
Coronavirus | Apr 4, 2020
COVID-19: Construction completed on first phase of Chicago's McCormick Place into Alternate Care Facility
Walsh Construction, one of the largest contractors in the city of Chicago and in the United States, is leading the temporary conversion of a portion of the McCormick Place Convention Center into an Alternate Care Facility (ACF) for novel coronavirus patients. Construction on the first 500 beds was completed on April 3.
Coronavirus | Apr 1, 2020
TLC’s Michael Sheerin offers guidance on ventilation in COVID-19 healthcare settings
Ventilation engineering guidance for COVID-19 patient rooms
Healthcare Facilities | Mar 29, 2020
A ‘roadmap’ for building hospitals in rural and underfunded markets
Hoar Construction’s formula emphasizes preconstruction planning and input from healthcare workers.
Healthcare Facilities | Mar 27, 2020
Designing healthcare for surge capacity
We believe that part of the longer-term answer lies not just with traditional health providers, but in the potential of our cities and communities to adapt and change.
Modular Building | Mar 17, 2020
Danish hospital is constructed from 24 steel frame modules
Onsite construction was completed in two weeks.
Healthcare Facilities | Mar 9, 2020
Mobile wayfinding platform helps patients, visitors navigate convoluted health campuses
Gozio Health uses a robot to roam hospital campuses to capture data and create detailed maps of the building spaces and campus.
Healthcare Facilities | Feb 28, 2020
Valleywise Health Medical Center breaks ground in Phoenix
Cuningham Group Architecture and EYP designed the project.
Healthcare Facilities | Feb 27, 2020
Milieu: Creating restorative environments in behavioral health
It’s time to take a closer look at the collection of therapeutic settings known as milieu.